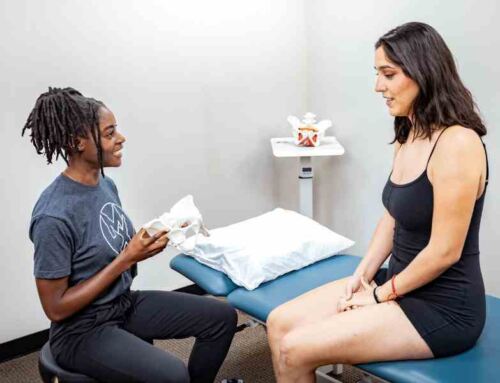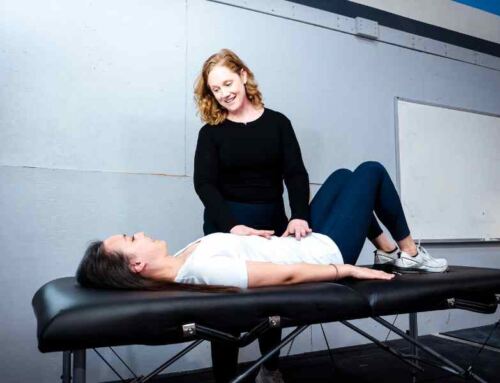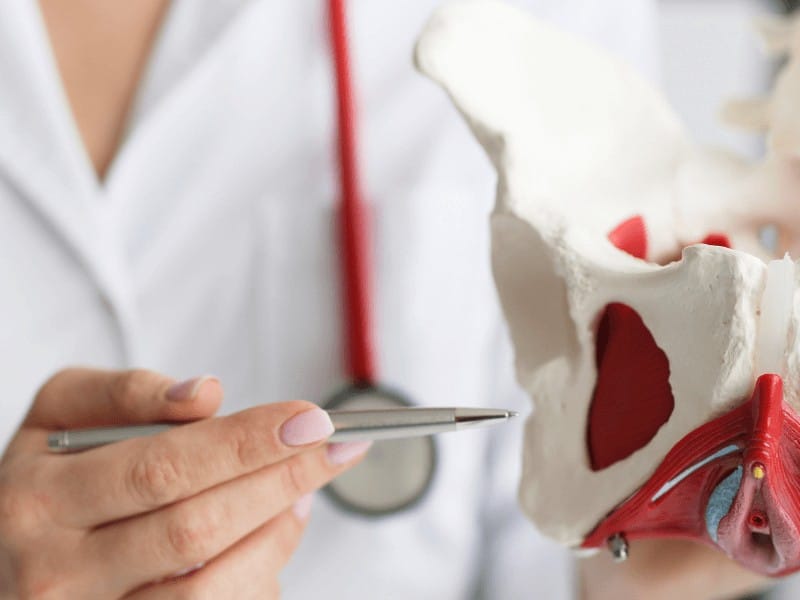
What Does Specialized Pelvic Floor Physical Therapy Look Like?
The conversation transcribed below originally aired on “The Point” KPOV 88.9. FM high desert community radio in Bend, Oregon.
Click here to listen along to the full radio show.
Our guest today is Mackenzie Van Loo, a physical therapist in Bend who specializes in the pelvic floor area. So you know, as women, as women age, there’s a growing focus on healing the pelvic floor region, whether it’s for sexual intimacy, or incontinence. And this isn’t always an easy subject to talk about, and for young women as well, they can struggle too. So our guest today is Mackenzie Van Loo, a physical therapist in Bend that focuses primarily on the pelvic floor region. So welcome to The Point, Mackenzie!
Hello, thank you so much for having me! It’s a pleasure to be here.
Yes, we’re excited. So Mackenzie, we had Dr. Carol Petherbridge, on our show, and she was talking about the very same issues. But I wanted to have you on because of your vast knowledge in this area. And the idea that, you know, a lot of people don’t know that physical therapy in the pelvic region can actually help women. So let’s dig in. Tell us what is pelvic floor physical therapy?
Great! Pelvic floor physical therapy refers to this subset or the sub specialty in orthopedics. So in doctor physical therapy school, we get permission to treat the entire body from an orthopedic and neurologic standpoint. After school, there are hundreds of hours of classes that you take in order to get permission to work on the pelvic floor. So just like everything else in your body needs to have strength, endurance, range of motion, coordination, and power, both locally and as a system.
Your pelvic floor is the exact same. I use my PT brain for strength, endurance, range of motion, coordination and power for helping people solve their issues around the pelvic floor. So things like urinary incontinence, urinary urgency and frequency, constipation, pain with sex, pain with orgasm, or even chronic pain, like in the back and hips that doesn’t really resolve or get better with normal classic PT.
How do you know when it becomes severe enough to need the therapy itself?
Oh, that’s a great question. I think there’s that old adage of an ounce of prevention is worth more than a pound of cure. Many times, especially… let’s use some low hanging fruit: Pregnancy is something that changes your body from the inside out. Getting to know how to use your pelvic floor before you become pregnant is actually really super helpful. I help people actually figure out how to push efficiently in labor, how to strengthen those muscles.
So we tend to say, if you leak any urine or have any loss of control of your pelvic content (so pelvic organ prolapse, you maybe have to rush to the bathroom for bowel or bladder, or you leak even just a little bit with a sneeze or a cough, or even with a PR deadlift), all that stuff is really common, but it doesn’t have to be normal. Now, I don’t want to ever spread a stigma that you should be ashamed of leakage, like common, but not normal can have some weird connotations. But if you feel like you don’t want to leak, you definitely don’t have to. You do not have to wait until it is “so bad” to get care.
You know, that’s great information, because, you know, I don’t know why it’s so hard for women to address it. You know, whether it be sexual intimacy or incontinence. Do you think the tide is turning a little bit now that where women are saying, you know, it’s not okay to leak it’s not okay to even young women not not be able to use a tampon or you know, or not be able to have a successful orgasm. I mean, do you think the tide is turning where women are okay to talk about this?
I think so. Yes. Like with change, like younger and younger generations being more and more okay with talking about things that you know, are taboo to some others. It definitely is changing the tide. Now, is it as fast as I’d like it to be? Probably not. But I think as people become more aware and become more comfortable. I think the tides are turning but again, not as fast as I would like.

So do you feel like a lot of people experience these problems with their pelvic area, but they are not aware of the solution of physical therapy, so they often go untreated?
Yes, actually, I should have refreshed my mind on statistics, but I believe it’s one in three women over the age of 65 have urinary incontinence, and I can confidently say that’s only 1/10 of pelvic floor dysfunction. That’s not counting all the other things that I’ve listed and more. Pain with sex is extremely prevalent, especially after having a baby. Or even as we age, our tissue dries, our pelvic muscles get tighter, and sex becomes painful. So yeah, it is actually extremely common.
Also, two out of five—something like that—of young athletes, like collegiate athletes actually leak. These are women who have not had babies. And men have pelvic floors, so they also leak and have pain with orgasm! They also have constipation, they also have all these issues.
Wow, now to this is why I really wanted to have you on because I found it really fascinating how physical therapy can work in the pelvic area. I mean, I know I’ve been in for my shoulders, and they move my shoulders and stretch my shoulders. And, you know, and I’ve been in for my hip and they, you know, do things. But can you just geek out a little bit and tell us how the nerves and muscles relate to the pelvic floor area? And why PT would be good for it.
Oh, thank you. I love this question! So the pelvic floor and think of it this way, your body is like a team. So just like you are a team with your co host, and your team in your family. Everybody has their roles to play and short term if we dropped the ball or we’re sick and someone else can kind of come along and help make up the slack. Long term, that’s when the person is taking up the slack, can get a little frustrated, a little extra tired, they start not doing well. That’s exactly how the body works. So your pelvic floor, its capacity to do its job is also dependent on all the other muscles and structures that attach on the pelvis.
So everything from your neck, and your jaw and your throat, all the way down to your big toe affects how your pelvic floor is able to do its job. You are 80% likely to have some form of pelvic floor dysfunction if you also have back pain, or hip pain. So anything that attaches onto the pelvis, like the hip, like your vertebra, like your abdominals, if they do not have appropriate strength, endurance, range of motion, coordination, and power locally, and then as a whole system, your pelvic floor many times is the last ditch effort. That team member that’s always trying to take up that extra work.
So pelvic floor physical therapy includes looking at those shoulders, looking at those hips, looking at the back, and making sure that the nerves, the bones, the joints, the muscles, everything works together as a team.
Is all of the work done on the outside? Or is some of the work done vaginally? Yeah, you know, or internally?
Perfect question. Yes. So part of becoming a trained pelvic floor physical therapist, I get permission to and significant training to assess the pelvic floor muscles externally. And internally, that’s either through the vagina, or through the rectum, depending on the problem. So tailbone issues would be through the rectum, constipation, lots of stuff through the rectum as well. But it also includes external, like we just said, and really thorough orthopedic assessment of the hip, the low back. the pelvis.
And before the show, you had mentioned that it is not common for people to be as specialized in the pelvic region as you are. Could you expand on that and why it’s important to have someone who’s super specialized to perform this kind of therapy?
Oh, yes, thank you. So yes, I am the only board certified women’s clinical specialist in Central Oregon, there’s only 12 of us in the state, and only a couple 100 of us in the whole United States. It’s just extra hundreds of hours, and then a big exam and a big case study that’s reviewed. So it’s just taking those extra steps to make sure that I have other people more advanced than I looking into my career and saying, “Are you doing the best for your patients?” Now, there are plenty of people that practice very well that do not have this certification. It’s just what I chose to do.
But doing these certifications, I also have my clinical specialty in Obstetrics and Gynecology, and that’s given me extra training to help someone prepare for birth and recover from birth and keep training during birth. I have my postpartum athleticism and pregnancy coach certification as well. So having more specialty means I’ve spent more time really critically thinking about the research and what is a science based way for me to help people. But again, not everybody needs super specialized care either, right? So it’s called a physical therapy practice. So like any medical practice, as we practice more in our careers, we get better and better. And so I just like to pursue knowledge a lot.
What do people say when you tell them what you do? I mean, what is the big question that people ask when you say this?
It always depends on the people in front of me. Most moms nowadays know what I do with pelvic floor PT in there, like, oh, I should come see you, which is super flattering. Now, if I’m with my husband’s co workers, and they ask what I do, most of them, because their engineers go, “oh, well, interesting.” And then the conversation switches. So it always depends on who’s in front of me, right? It can be very taboo.
There’s this really uncomfortable stigma that my job is somewhat sexual, where we do talk about sexual health in a very, very matter of fact, and informative way. But yeah, a lot of people have some really strange connotations around the work that we do. But I think it’s justice work. Our capacity to feel like adults and human beings has a lot to do with our capacity to control urine,l bowel, and have pain free intimacy, with the people we care about. And that’s why I do what I do. That is great.

And we’re back. I’m Jackie Elliot here with my co host, JC silk. And she’s sitting in for Carolyn esky on the Friday edition of the point. And we’re continuing our conversation with physical therapists Mackenzie Van Loo. She specializes in pelvic floor therapy. So we’ve been having a wonderful talk backstage here as they say in the greenroom. But you know, one of the things I wanted to bring up was pelvic floor therapy for trans for the trans population for children and for men. I know we’ve been talking about women’s issues. Tell us a little bit about those issues that you deal with.
Yes, thank you. So everybody has a pelvic floor. The pelvic floor tends to get a lot of press for people who are pregnant or have babies or want to have babies.
But also just individuals who are struggling with gender dysphoria. People who are unhappy with their body, people have had sexual trauma, people have had prostatectomies, even young children who bedwet late into childhood, all of those things are something pelvic floor physical therapists can help with, especially ones that have advanced training, and are of course comfortable treating those specialty populations. I say specialty populations, because that’s what the physical therapy groups say. I think that they should not be specialty, they should be basic, right? Everybody has a pelvic floor. Everyone deserves to have care and not have difficulty with orgasm, pain with intercourse, or significant post surgical pain.
So post bottom surgery, post gender affirming surgeries, the surgeries are absolutely amazing and intricate. And these people need physical therapy. It’s painful. And so I pride myself in being able to help people with that. It’s a privilege to help trans individuals recover and feel more at home in their bodies.
Well, you know, about children bedwetting, a lot of parents are concerned about that. How would you treat a child who bed wets?
Most of the time, it’s not always but a large majority of the time children who bed wet late into childhood are actually constipated. So if you think about the pelvis, it is a really small container, and it holds the bladder, uterus, for those who have a uterus and your rectum. Your rectum and your bladder are very close. If your rectum is full of hard poop, can you imagine how that would really encroach on space on the bladder. And just holding that toxic stuff inside your body will also just up regulate your nervous system and make it harder to control urine.
So treating kids a lot of the time have we use biofeedback externally, or I actually use lumbopelvic real time ultrasound. So I’ll use a very friendly little ultrasound wand like what people used to look at ultrasounds for babies. We put that on their tummy and we can actually measure the rectal diameter and know what’s normal, and see if they are full of poop. And then we work really closely with their doctor or their primary care to help them get cleaned out, get them in their parents on a schedule for helping train them if their sensory processing disorders we also get OT involved. Yeah, it’s again holistic, a big picture for treating kids. I love real time ultrasound, it makes treating them so much easier. Because yeah, can be kind of intimidating to do PT, especially for the kids.
Yeah, I did not know all of that. But how is treating men different than treating women?
Well, for those that identify as male, there’s, again in our society, a lot of a lot of things we grew up with, right? A lot of things that tell us who we are and whether or not it’s okay to talk about things. And I think generally as women are okay, more okay with talking about medical issues than maybe some of our male counterparts. So treating men is different in that we have the privilege of teaching them about their body in a way that’s never really talked about very often.
And treating men, I treat a lot of people with erectile dysfunction, teaching people how to care for their tissue after a prostatectomy to help them not leak, but also help them regain the capacity to have erections. Yeah, lots of stuff. But I mean, I see men for all the same things I see women for and all the same things I see trans individuals for: bowel issues, bladder issues, constipation, hemorrhoids stuff. Yeah. All of it. All of it.
Well, I know JC you had mentioned that you had known a friend who had received the therapy, and had an experience with that.
Yeah, she actually had tremors around the pelvic floor. And then she received three sessions of pelvic massages. And afterwards, it was quite painful for her. So I was wondering, does pain often go hand in hand with the therapy, even though she did receive relief for her problem after? How does that affect people who received the therapy?
Yeah, so I’m not of the school that says, “No pain, no gain,” for pelvic floor rehab. And while there are times such as in tendon rehab, yeah, pain is definitely part of rehab, the pelvic floor and the pelvis, is a really intimate area. Significant pain should not be a normal piece of this type of rehab. And even when people have pain with gynecological exams, or pain with a tampon insertion, pain during rehab should always be tolerable. It should always be tolerable and should never really pay for it afterwards. There are times where I do prep patients for that. But generally, there are advanced manual therapy ways that we can treat people and really put their nervous system at ease cognitively but also physically to help down regulate the nervous system so pain is almost not a factor at all.
One thing that you also mentioned is you get a lot of questions related to kegels, is this equivalent to pelvic therapy? Or what are your comments on that?
Thanks for bringing that up. Yes. So many times I say, Oh, I’m the pelvic floor physical therapist, like, “Oh, I do my kegels, I’m good.” And I am of the thought that unless you literally just gave birth to a baby, or have a ton of pelvic floor length. You know, doing kegels is actually not pelvic floor physical therapy, there is maybe 10% of my practice where I will prescribe them.
Pelvic floor rehab actually has to do with treating your whole system, like we talked about making sure your abs, your low back, your butt, all the other big muscles that are meant to locomote you through your day, those things actually need to be trained, there’s really great and really clear evidence to show that if we just get your whole body strong, your pelvic floor will do its job. We just have to be smart about it. So yeah, it’s definitely more than just kegels. And if you ever have gone to therapy, and only have done kegels, and only been on your back the whole time and you didn’t get what you wanted results wise… It’s always worth looking elsewhere. Yeah, it’s more than just kegels.
Well, you know, I just we don’t we’re running out of time, we have about a minute left. But I just want to say that I have, you know, full disclosure, I’ve been to Mackenzie. And the way you practice is so safe and so comfortable. I want to assure people who are maybe afraid or feel like, you know, scared by this that Mackenzie makes it very, very comfortable and explains everything so that it’s just, it all makes sense. So we can see. In this next minute we will tell people how they can get a hold of you and how they can learn more information about this.
Thank you so you can find me on Instagram. I am the @Sanctumphysio on Instagram, you can also find me through movement-x.com I am the only person in Bend practicing and contracting my LLC through MovementX. I’m accepting new patients, I’ve opened my own business and I go to people’s homes where they can be more at ease. And I also have a private treatment space in my own home. And I just take a lot of pride in and and I feel very privileged to do what I do for Central Oregon. So Jacquie, thank you for sharing your experience with me. It is so meaningful to have that feedback. It’s just a pleasure to be here.
Yeah, so one more time, that email or website…
You can find me @Sanctumphysio on Instagram and Movement-X.com.
Thanks for listening to this KPOV podcast.
About the Author
Mackenzie Van Loo, PT, DPT is a physical therapist and pelvic health specialist in Bend, OR. She is a Board Certified Women’s Clinical Specialist (WCS) and has a certificate of achievement in Obstetrics (CAPP-OB). Mackenzie aims to provide exceptional service rooted in wisdom and intention to combat the physical injustices of this world. Click below to request a session with her today.