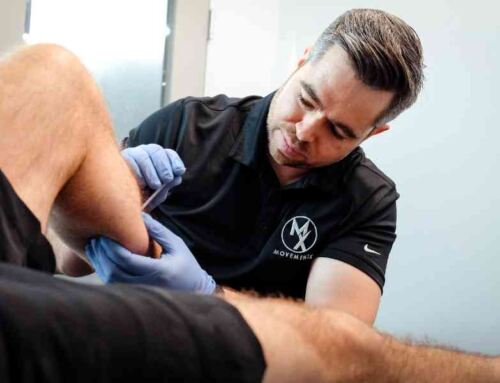
If you’ve spent any time in EDS support groups or scrolling social media, you’ve seen the extremes. On one side, there are terrifying lists of “10 things you should NEVER do if you have EDS.” On the other, there are posts promising that “these 5 stability exercises” are the magic key to fixing your joints. And yet somehow, physical therapy (the one place that’s supposed to cut through all of that) often just hands EDS patients another list.
In physical therapy, there’s a joke that the answer to every question is: “it depends.” But for some reason, when it comes to hypermobility, that nuance often disappears. Many patients find themselves trapped in a cycle of “safe” but ineffective rehab. You might be told to “protect” your joints by avoiding movement, or be given the same basic “Level 1” exercises regardless of whether you’re a high-level athlete or someone just trying to get through a workday without a flare.
The truth is you can’t protect your way into a higher functional state. Real care isn’t about following a rigid protocol; it’s about finding your specific entry point. The place where we challenge your body just enough to help it adapt, without pushing it over the edge.
But it’s so confusing! You leave your doctor’s office having been told to be very careful to not hurt yourself. But they also tell you to go exercise to get better with no guidance on how to be careful nor how to exercise.
As a patient, I’ve been given this advice before and it’s what drives me to do better for my own patients. So, let’s talk about the things that are better than the norm when working with a physical therapist for your EDS. It’s neither about being perfectly comfortable, nor being asked to do the impossible. It’s about a relationship where you feel like you’re being challenged to make meaningful progress that’s specific to your needs.
Here’s how it shakes out.
The Value of a Thorough Assessment (Not Just a Checklist)
When you walk into a clinic, the assessment shouldn’t just be about how far your joints bend or a Beighton score. A diagnosis of EDS is a piece of the puzzle, but it isn’t the whole picture. To get you back to the things you love, we have to start with one simple question:
What are your goals?
If your goal is to run a marathon and your PT has you doing three sets of ten leg lifts on a table, there is a specificity gap. Those table exercises might be “safe,” but they aren’t preparing your tissues for the impact of the pavement.
Your marathon might actually be something more like standing in the kitchen to cook a meal for your family, picking your toddler up and putting them in the carseat, or just getting through the workday.
No matter your goal, your plan of care needs to be specific to you and what you want to do. Because otherwise, what’s the point? I don’t know about you, but I don’t particularly care how many clamshells I can do on a treatment table if it’s not helping me live my life off the table.
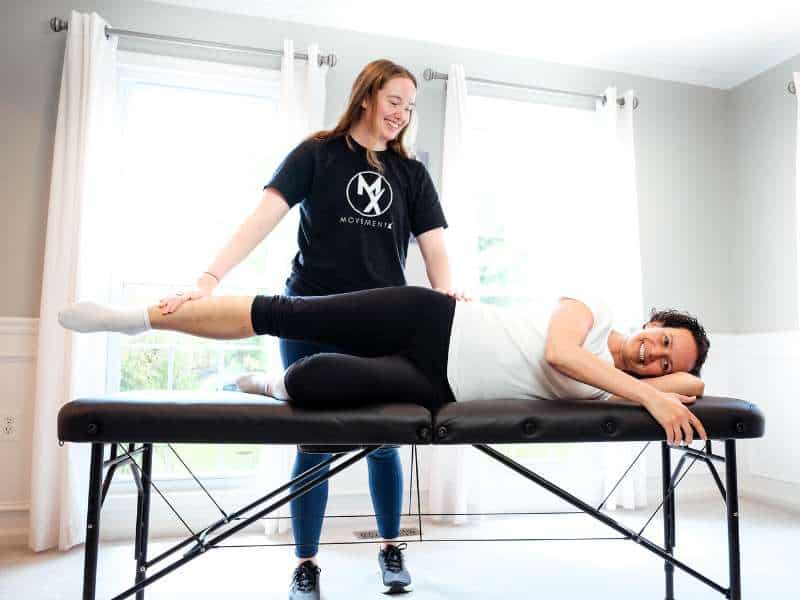
Finding Your “Mechanical Entry Point”
I recently worked with a runner who was told she should never run or lift heavy again because of her hEDS diagnosis.
Her previous physical therapist was so afraid of over doing it that they never actually looked at what was causing her pain. She didn’t have pain while lying on a table; she had pain 2.5 miles into a run.
By only giving her “safe” low-level exercises, that therapist was actually under-dosing her. We didn’t need to protect her from the gym; we needed to find her current capacity and build from there.
This is what I call a Movement Audit (thank my accountant parents for the nomenclature).
Instead of banning a movement, we break down the movements you want to do. Take, for example, doing a squat.
We wouldn’t say “don’t squat” because you (likely) actually performed a squat to sit down and read this article without even thinking about it. Instead:
- We look at how you squat. Is the pain at the very bottom? Does it happen after 5 reps or 20?
- We adjust the variables. Maybe we slow down the movement, change the range of motion, or adjust the weight.
- We treat your environment. If we look at the actual needs imposed on you by your surroundings, what are the thresholds for success?
This is why I treat patients in their own homes or gyms. We aren’t guessing how you lift your toddler or use the squat rack; I am there with you, adjusting things in real-time on the equipment and in the space you actually use.
We aren’t looking for what’s “wrong” with you; we’re looking for what you can do right now, so we can expand that circle until it covers everything you want to do.
And some general principles can be applied across the board here.
We start low and slow, working up until we find a threshold we can work to improve.
We assess your actual range and capability. From there, we move deliberately towards the actual abilities you want to cultivate. Safely, through gradual exposure.
The Safety Paradox
Avoiding load can be risky for those with EDS.
We often talk about the fear of “over-doing it” with EDS. The dreaded flare that can set you back days or weeks. That fear is real and valid. It’s why physical therapy has to be a partnership with feedback going both ways to determine the best approach.
But we don’t talk enough about the opposite: The clinical risk of under-dosing.
If your physical therapy never reaches the threshold of your daily life, your body has no reason to adapt. Think of it this way: if you need to lift a 30lb toddler but your rehab only involves 1lb bicep curls, you aren’t being protected… you’re being unprepared.
Movement provides us with information we can use to calibrate our approach. And when we have the right type (and amount) of structured stress, you give your body (and your PT) the data needed to get stronger and more stable.

Contextual Loading
One of the reasons I chose a mobile model for my practice is because hypermobility doesn’t happen in a vacuum. It happens in your kitchen, at your desk, rolling over in bed, and at your gym.
In a traditional clinic, a PT is often just guessing. I might ask how you lift a heavy box, but I’m not seeing the specific height of your shelves or the exact grip you use. By treating you in your own environment (at home, in office, or wherever you want), we practice contextual loading:
- Real-time adjustments: We aren’t “simulating” a squat; we are using the actual rack and barbell you use every Tuesday and the laundry basket you use every Wednesday.
- Environmental variables: We can adjust the height of your office chair or the way you reach for your gear right where the “load-capacity mismatch” actually occurs.
- Precision dosing: We find the exact intensity that challenges you without pushing you over your symptomatic threshold because we are working in your real-world context with real-time feedback and conversation.
From Gatekeeper to Guide
For too long, the medical world has acted as a “Gatekeeper” for the EDS community. Telling you what you can’t do, where you can’t go, and which movements are “forbidden.”
I view my role differently. I am your Guide.
My job isn’t to give you a “safe” list of five exercises and send you on your way. My job is to help you build a blueprint that evolves as you do. An intervention is only “correct” if it prepares you for your actual life. Whether that’s running a marathon, sitting through a long meeting without pain, or playing with your kids, your goals are the compass for care.
The diagnosis is the starting point, but your capacity is a moving target. Let’s start moving it forward.
What to Do Next
If you’ve felt stuck in “rehab limbo,” you don’t have to stay there. Here’s how you can use this info and approach to change your outcomes:
1. Advocate for yourself
Take these concepts to your current provider. Ask them: “What is MY specific ‘entry point’ for this movement?” or “How does this table exercise prepare me for [your specific goal]?” A good clinician will welcome the chance to bridge that specificity gap with you. And if your symptoms fluctuate day-to-day, this has to be an ongoing open conversation.
2. Audit your environment
Pay attention to where your symptoms actually start. Is it at a certain weight? A certain time of day? A specific chair? Start tracking the context of your pain so you can bring that data to your next session.
3. Build your blueprint
If you’re tired of just protecting and are ready to start preparing, I’m here to help. I specialize in meeting EDS patients exactly where they are (literally), and you can reach out to me here.
Whether in your home or your gym, we will find your current capacity and build a plan that actually meets the demands of your life.
About the Author
Dr. Morgan Groover is a physical therapist based in Chantilly, VA. She treats pelvic health, orthopedic conditions, post-operative care, active adults and athletes, individuals with hypermobility, and people with POTS. As a former swimmer and current practitioner of an active lifestyle herself, Dr. Morgan Groover is ready to help you move better, live well, and get back to doing what you love.