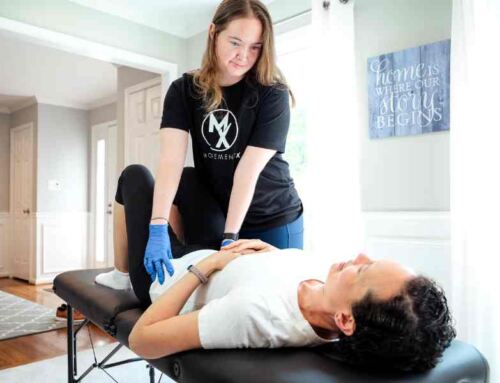
As a physical therapist, people almost always come to me because something hurts. It might be low back pain, neck tension, headaches, shoulder pain, or a knee that just won’t settle down.
Most people expect that we’ll identify a tight muscle, a weak area, or a joint that isn’t moving well… and sometimes that’s exactly what it is. A straightforward musculoskeletal problem with a clear physical solution.
But more often than not, the story is a little more complex.
Over the years, I’ve learned that when someone reaches out to me with physical pain, there is often more going on beneath the surface. The body rarely operates in isolation from the rest of our lives. Our stress, sleep, emotional health, and daily habits all influence how our body feels and functions.
That’s why some of my most important questions have nothing to do with the injured body part.
I often ask things like:
- How well are you sleeping?
- Have you had any significant stressors recently?
- How is your diet?
- What has your workload or daily life looked like lately?
Sometimes the answer reveals a lot more than expected. Maybe their gastrointestinal system hasn’t been functioning like it normally does. Maybe they’ve been under a heavy workload for months without much rest. Sometimes they share that they recently lost a loved one, went through a major life transition, or are navigating a particularly stressful season of life.
These things matter more than most people realize when it comes to physical pain.

The Nervous System Connects Everything
Our nervous system is constantly interpreting signals from both the body and the environment. When we experience prolonged stress, anxiety, emotional strain, grief, or poor sleep, the nervous system can remain in a heightened state of alertness.
In this state, the body becomes more protective and more sensitive.
Muscles may hold more tension. Pain signals may be amplified. Recovery from physical activity can slow down. Even movements that should feel normal can begin to feel uncomfortable.
Modern pain science supports this idea. Research shows that stress and pain share overlapping neural pathways in the brain, meaning emotional stress can directly influence how the body processes pain signals (Zheng et al., 2019). In other words, the brain doesn’t completely separate emotional stress from physical stress.
This doesn’t mean the pain isn’t real. In fact, it’s very real. It simply means that the nervous system is responding to more than just tissue strain.
Where Stress and Emotional Pain Show Up Physically
Many people carry emotional stress in predictable areas of the body.
The neck and shoulders often tighten during periods of mental overload or anxiety.
The jaw may become sore from clenching or grinding.
The low back can become sensitive when the body stays in a prolonged protective state.
Breathing patterns may shift to shallow chest breathing instead of relaxed diaphragmatic breathing.
Digestive changes can also appear during times of stress, since the nervous system that regulates digestion is closely tied to our stress response.
Psychiatrist Bessel van der Kolk famously described this concept in his book The Body Keeps the Score, explaining how emotional experiences, trauma, and chronic stress can manifest physically in the body.

Sleep and Pain Sensitivity
Sleep is another factor that plays a powerful role in how we experience pain.
Research shows that even short-term sleep deprivation can increase pain sensitivity by altering activity in the brain’s pain-processing centers and reducing the brain’s ability to regulate pain signals (Walker, 2019; Harvard Health Publishing). In other words, when we aren’t sleeping well, our nervous system becomes less resilient.
This is one of the reasons sleep is often one of the first things I ask patients about when we’re trying to understand persistent pain.
Piecing Together the Bigger Picture
When someone comes to me with pain, our first step is always to understand the physical side of the problem. Together, we try to piece things together: how the pain started, what movements reproduce it, what seems to aggravate it, and what helps relieve it.
From there, we work on improving the pain through movement, corrective exercise, and hands-on treatment. Restoring mobility, improving strength, and helping the body move more efficiently are essential parts of the process.
But many times, as we work through the physical side of things, other patterns begin to emerge. Sleep quality, stress levels, digestion, work demands, and emotional stress can all influence how the body is responding.
That’s where a whole-person approach becomes important.
A Collaborative, Whole-Person Approach
While physical therapy plays a major role in helping people move and feel better, there are limits to what any single provider can do on their own. Pain and health are multifaceted, and sometimes the best outcomes happen when multiple areas of health are addressed together.
If emotional stress, anxiety, or grief seem to be playing a significant role, I often encourage patients to speak with a psychotherapist or mental health professional. Processing emotional stress and learning tools for regulation can have a powerful impact on the nervous system and in turn, on physical symptoms.
For people who want tools they can begin using right away, practices like meditation, mindfulness, and breathing exercises can also help calm the nervous system and reduce physical tension.
Nutrition is another important piece. If diet or digestive issues seem to be contributing to inflammation, low energy, or poor recovery, I often recommend working with a registered dietitian who can provide individualized guidance.
And when questions arise around hormones, gut health, lab work, or broader medical concerns, I often refer patients to a functional medicine physician or another medical provider who can look deeper into those systems. A provider I frequently refer to in the Knoxville area is Emily Turner at Omni Functional Medicine.
“In medicine we often see that the body expresses what the mind and nervous system have been carrying for a long time. Chronic stress, trauma, and emotional strain can manifest as physical symptoms like pain, fatigue, inflammation, and digestive issues. When we begin addressing both the emotional and physiological roots of illness, patients often experience deeper and more sustainable healing.”
Emily Turner PA-C, Omni Functional Medicine
This collaborative approach allows each professional to work within their expertise while supporting the patient as a whole.

The Takeaway
The body is remarkably intelligent. It reflects not only how we move but also how we live, cope, and recover.
People usually reach out to a physical therapist with a physical complaint, and sometimes that’s exactly what it is. But many times, the body is also carrying the effects of stress, fatigue, emotional strain, grief, and lifestyle habits.
By addressing the physical side of pain while also considering sleep, stress, nutrition, digestion, and emotional health, we can start to see the bigger picture.
Because sometimes the most important question isn’t just “Where does it hurt?”
It’s “What else might your body be trying to tell us?”
References
- Zheng, G., et al. (2019). Chronic stress and pain: Neural mechanisms linking stress and pain processing. Neuroscience & Biobehavioral Reviews.
- Walker, M. (2019). Sleep loss and pain sensitivity research findings. Journal of Neuroscience.
- Harvard Health Publishing. Poor sleep can change your reaction to pain.
- van der Kolk, B. (2014). The Body Keeps the Score: Brain, Mind, and Body in the Healing of Trauma.
About the Author
Dr. Ashton Grimm is a physical therapist and certified Orthopedic Specialist in Knoxville, Tennessee. Among Ashton’s treatment specialties are orthopedics, sports, neurologic, geriatrics, and vestibular conditions. Dr. Ashton works with a wide range of individuals, from athletes and runners to working moms, active grandparents, and young professionals, helping you stay mobile, independent and pain-free.